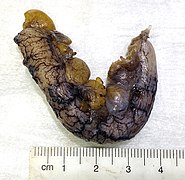
Appendicitis
Jump to navigation
Jump to search
Author:
Mikael Häggström [note 1]
Appendicitis may histopathologically be defined as neutrophilic infiltrates of the wall of the appendix in the correct clinical context.
See also: General notes on fixation
Contents
Comprehensiveness
On this resource, the following formatting is used for comprehensiveness:
- Minimal depth
- (Moderate depth)
- ((Comprehensive))
Gross processing
Standard sections if the appendix appears inflamed and there are no signs of malignancy. Describe abnormal signs including:
Further information: Appendix
Microscopic evaluation
- Evaluate depth of the inflammation.
- Look for any perforation of the wall.
- Look for cancerous cells (which may have caused the appendicitis). Further information: Appendix
- (Attempt to specify the type of appendicitis as either of the following:)
Types
| Pattern | Gross pathology | Light microscopy | Image | Clinical significance |
|---|---|---|---|---|
| Acute intraluminal inflammation | None visible |
|

|
Probably none |
| Acute mucosal inflammation | None visible |
|
May be secondary to enteritis. | |
| Suppurative acute appendicitis | May be inapparent.
|
|

|
Can be presumed to be primary cause of symptoms |
| Gangrenous/necrotizing appendicitis |
|
|

|
Will perforate if untreated |
| Periappendicitis | May be inapparent.
|
|

|
If isolated, probably secondary to other disease |
| Eosinophilic appendicitis | None visible |
|
Possibly parasitic, or eosinophilic enteritis. | |
| Chronic appendicitis[2] |
|
|
Should preferably correlate with long-term or recurrent symptoms. |
Further workup
(In acute suppurative appendicitis, still look for any periappendicitis. Also look by the lumen for parasites.)
Microscopy report
Should include, if detected:
- Acute or chronic appendicitis
- Depth of inflammation
- Any abscess and\or perforation
- Necrosis and\or ulceration, at least if transmural
(Classification into one or several types as per table above.)
- Example
| (Appendix, resection (or appendectomy):) Acute (suppurative) appendicitis (and periappendicitis) with transmural necrosis and perforation. |
Notes
- ↑ For a full list of contributors, see article history. Creators of images are attributed at the image description pages, seen by clicking on the images. See Patholines:Authorship for details.
Main page
References
- ↑ Unless otherwise specified in rows, reference is:
- Carr, Norman J. (2000). "The pathology of acute appendicitis ". Annals of Diagnostic Pathology 4 (1): 46–58. doi:. ISSN 10929134. - ↑ Sierakowski, Kyra; Pattichis, Andrew; Russell, Patrick; Wattchow, David (2016). "Unusual presentation of a familiar pathology: chronic appendicitis ". BMJ Case Reports: bcr2015212485. doi:. ISSN 1757-790X.
Image sources