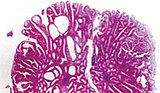
Colorectal polyp
Author:
Mikael Häggström [note 1]
| Mostly: |
Contents
Gross examination
Further information: Colon
Tissue selection and trimming

Depending on sample format:[1]
- Biopsies and polyps of <4 mm are embedded in their entirety. Samples less than 0.3 mm should be stained with eosin to avoid getting lost processing.
- Polyps 4-8 mm with short stem or without stem: Identify the excision surface and divide the polyp longitudinally through the excision surface.
- Polyps > 8 mm with a stem long enough to make it possible to take a transverse, whole slice from the stem closest to the excision surface: First, take a transverse slice through the peripheral portion of the stem, encompassing the entire circumference. Then take a 3-4 mm thick slice longitudinally through the polyp and the middle of the stem, after which the two remaining parts on either side are cut into equally thick slices, parallel to the previous slice.
- Polyps >8 mm with short stem or without stem: Identify the excision surface and cut out a 3-4 mm thick disk that extends longitudinally through the center of the excision surface. Then divide the two remaining portions into equally thick slices, parallel to the previous slice.
- Polyps that come in parts: Pick out the largest pieces, which are cut as similar as possible to above. Small fragments are sieved and embedded in a separate box.
Gross reporting
- Polyp and/or fragment sizes
- Presence or absence of stem of polyps
Example, for a gastrointestinal biopsy:
| Labeled: "Sigmoid colon biopsy". The specimen is received in formalin and consists of 4 fragments of pink-tan tissue with a vaguely recognizable mucosal surface, mixed with food-like material. The fragments measure 0.2-0.3 cm in greatest dimension. The entire specimen is submitted for microscopic examination in one cassette. |
Microscopic evaluation
Major signs
Look particularly for these, to help sorting into proper diagnosis in next section:
Main types
Consider at least the following conditions:

| Type | Risk of containing malignant cells | Histopathology | Image | |
|---|---|---|---|---|
| Hyperplastic polyp | 0% | No dysplasia.[3]
|

| |
| Tubular adenoma | 2% at 1.5cm[5] | Low to high grade dysplasia[6] | Over 75% of volume has tubular appearance.[7] | 
|
| Tubulovillous adenoma | 20% to 25%[8] | 25%-75% villous[7] | 
| |
| Villous adenoma | 15%[9] to 40%[8] | Over 75% villous[7] | 
| |
| Sessile serrated adenoma (SSA)[10] |
|

| ||
| Traditional serrated adenoma | 
| |||
| Colorectal adenocarcinoma | 100% |
|

| |
If you only see normal mucosa but the order/endoscopy says polyp, take additional levels from the paraffin block.
Other benign
If a more specific diagnosis cannot readily be made, clearly non-malignant colorectal polyps may simply be reported as such.
- Further information: Evaluation of tumors
Microscopy report
It should include:[12]
- Size of polyp (from gross examination)
- Histopathologic type
- Depth of growth and/or infiltration
- Whether the resection is radical
Optionally, it can include degree of differentiation and/or dysplasia.
Example:
| 50 mm large tubulovillous adenoma with up to high grade columnar epithelial dysplasia. No infiltration. Radical excision. |
If multiple polyps are submitted in one container, you may count the amount of each polyp type if you can, but if the amount of fragments in microscopy exceeds the amount of fragments purportedly submitted, then you can simply write "fragments of", like the following example:
| Fragments of tubular adenoma and hyperplastic polyp. |
More details are given in main articles of histopathologic types.
See also: General notes on reporting
Notes
- ↑ For a full list of contributors, see article history. Creators of images are attributed at the image description pages, seen by clicking on the images. See Patholines:Authorship for details.
Main page
References
- ↑ Monica Dahlgren, Janne Malina, Anna Måsbäck, Otto Ljungberg (1997-02-13). Lilla utskärningen.
- ↑ References for pie chart are located at separate image description page.
- ↑ 3.0 3.1 3.2 Finlay A Macrae. Overview of colon polyps. UpToDate. This topic last updated: Dec 10, 2018.
- ↑ 4.0 4.1 4.2 Robert V Rouse (2010-01-31). Hyperplastic Polyp of the Colon and Rectum. Stanford University School of Medicine. Last updated 6/2/2015
- ↑ Minhhuyen Nguyen. Polyps of the Colon and Rectum. MSD Manual. Last full review/revision June 2019
- ↑ Robert V Rouse. Adenoma of the Colon and Rectum. Original posting/last update : 1/31/10, 1/19/14
- ↑ 7.0 7.1 7.2 Bosman, F. T. (2010). WHO classification of tumours of the digestive system . Lyon: International Agency for Research on Cancer. ISBN 92-832-2432-9. OCLC 688585784.
- ↑ 8.0 8.1 Amersi, Farin; Agustin, Michelle; Ko, Clifford Y (2005). "Colorectal Cancer: Epidemiology, Risk Factors, and Health Services ". Clinics in Colon and Rectal Surgery 18 (03): 133–140. doi:. ISSN 1531-0043.
- ↑ Alnoor Ramji. Villous Adenoma Follow-up. Medscape. Updated: Oct 24, 2016
- ↑ Rosty, C; Hewett, D. G.; Brown, I. S.; Leggett, B. A.; Whitehall, V. L. (2013). "Serrated polyps of the large intestine: Current understanding of diagnosis, pathogenesis, and clinical management ". Journal of Gastroenterology 48 (3): 287–302. doi:. PMID 23208018.
- ↑ 11.0 11.1 11.2 11.3 Enoch Kuo, M.D., Raul S. Gonzalez, M.D.. Colon - Polyps - Traditional serrated adenoma. Topic Completed: 1 February 2018. Minor changes: 1 October 2020
- ↑ Monica Dahlgren, Janne Malina, Anna Måsbäck, Otto Ljungberg. Stora utskärningen. KVAST (Swedish Society of Pathology). Retrieved on 2019-09-26.
Image sources