Gross processing of skin excisions
Author:
Mikael Häggström [note 1]
Contents
Comprehensiveness
On this resource, the following formatting is used for comprehensiveness:
- Minimal depth
- (Moderate depth)
- ((Comprehensive))
Frozen sections
Melanocytic lesions will look atypical by artifacts on frozen sections, limiting its value in for example clearing margins.
Submission of entire specimen
Serial sectioning and submission of the entire specimen is recommended when the referral or clinical history indicates a pertinent lesion, but no lesion is grossly visible.[1]
((Also, submit the entire specimen for suspected malignant skin excisions when the distance from the lesion edge to the tip does not exceed about 2-3 cm in either direction. Have a longer threshold for suspected melanomas.))
Partial submission of specimen
The rest may be saved in case microscopy indicates further sampling.
Lens-shaped excisions
Also called marquise ("lens" or "boat") shape.[notes 1]
| Lesion size | |||
|---|---|---|---|
| <4 mm | 4 - 8 mm | 9 - 15 mm | |
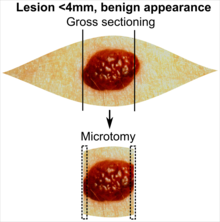
| Benign appearance | |||
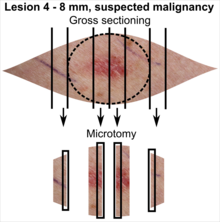
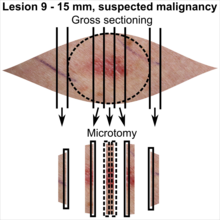
| Suspected malignancy | 
|
|
|
In table above, each top image shows recommended lines for cutting out slices to be submitted for further processing. Bottom image shows which side of the slice that should be put to microtomy. Dashed lines here mean that either side could be used.
Oval excisions
These can often have a parallel radicality cut along each lateral edge.[3]
Wedge-shaped excisions
Two alternatives shown at above for excisions over 8 mm.[4] If the excision is very irregular at the edges, making a whole slice from the resection surface impossible, take parallel vertical or horizontal slices.[4]
Radicality slices
| In situ | 5 mm |
| ≤ 2.0 mm | 1 cm |
| > 2.0 mm | 2 cm |
The example shown for suspected malignancy risks has parallel slices to check for radicality towards the tips.[2] They are placed at a distance to provide similar margins as the shortest one in the short axis. However, if the shortest margin is narrower than recommended (such as less than 4 mm for a suspected squamous cell carcinoma)[6], consider expanding the distance towards the tips by taking more slices or sections:[notes 2]
Microtomy should start at the most central surface, leaving the option to perform further microtomy for radicality on the same slice in case the first one shows tumor cells. However, if tumor cells are found near the resection margins on the radicality slices, non-radicality cannot be excluded by additional sampling towards the tips.
Gross margin measurements
These are generally not needed, unless the skin excision is big enough to not conveniently include both the lesion and the nearest margin.
Wounds
Measure both the area and depth of the wound (if applicable). Take a radial section of the wound, including adjacent viable tissue. Radicality is not important unless specifically requested. If calciphylaxis is included as a target, sample approximately 1 slice per cm of tissue.
Inking
If the sample is marked with one or more sutures or colored nails, perform inking of one or both of the sides, from one tip to another, and document how the inking relates to any markings before removing them.[7]
The example at right shows a minimal amount of ink colors, necessitating that each radicality slice is submitted in a separate cassette.
For wedge-shaped skin excisions, apply ink to both surgical edges.[4]
Report
- Patient and/or sample data
- Optionally, location
- Size of sample
- If any focality, report its:
- Size
- Color
- Sharp or diffuse border
- Any elevation
- How inking was done, and how it relates to any markings.[7]
- How much is submitted (such as "entire sample" or "entire lesion")
- Contents of each submitted block
Example:
|
Sample #15315 Joe Bloggs 2000-01-01
|
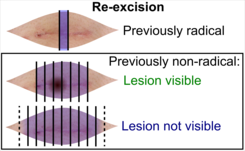
Re-excisions
((Submit the entire specimen, or)) depending on radicality of previous excision:
- Previously radical (including thin margins): Submit at least one central section across the surgical scar.[8]
- Previously non-radical:
Notes
- ↑ For a full list of contributors, see article history. Creators of images are attributed at the image description pages, seen by clicking on the images. See Patholines:Authorship for details.
- ↑ The excision examples show a normal mole (upper row, benign appearance) and a superficial basal cell carcinoma (lower row, suspected malignancy).
Main page
References
- ↑ Singh, ManojKumar; Ranjan, Richa; Singh, Lavleen; Arava, SudheerK (2014). "Margins in skin excision biopsies: Principles and guidelines ". Indian Journal of Dermatology 59 (6): 567. doi:. ISSN 0019-5154.
- ↑ 2.0 2.1 There are many variants for the processing of skin excisions. These examples use aspects from the following sources:
- . Handläggning av hudprover – provtagningsanvisningar, utskärningsprinciper och snittning (Handling of skin samples - sampling instructions, cutting principles and incision. Swedish Society of Pathology.
- For number of slices and coverage of lesions, depending on size. - Monica Dahlgren, Janne Malina, Anna Måsbäck, Otto Ljungberg. Stora utskärningen. KVAST (Swedish Society of Pathology). Retrieved on 2019-09-26.
- For slices towards the tips to determine radicality, which can be parallel to the slices through the lesions (shown), or as longitudinal slices that go through each tip. - . Dermatopathology Grossing Guidelines. University of California, Los Angeles. Retrieved on 2019-10-23.
- For microtomy of the most central side at the lesion - "The principles of mohs micrographic surgery for cutaneous neoplasia
- With a "standard histologic examination" that, in addition to the lesion, only includes one section from each side along the longest diameter of the specimen.
- It also shows an example of circular coverage, with equal coverage distance in all four directions.
- The entire specimen may be submitted if the risk of malignancy is high. - . Handläggning av hudprover – provtagningsanvisningar, utskärningsprinciper och snittning (Handling of skin samples - sampling instructions, cutting principles and incision. Swedish Society of Pathology.
- ↑ Katarzyna Lundmark. Handläggning av hudprover – provtagningsanvisningar, utskärningsprinciper och snittning (Handling of skin samples - sampling instructions, cutting principles and incision. Swedish Society of Pathology.
- ↑ 4.0 4.1 4.2 . Handläggning av hudprover – provtagningsanvisningar, utskärningsprinciper och snittning (Handling of skin samples - sampling instructions, cutting principles and incision. Swedish Society of Pathology.
- ↑ Shenenberger DW (2012). "Cutaneous malignant melanoma: a primary care perspective. ". Am Fam Physician 85 (2): 161-8. PMID 22335216. Archived from the original. .
- ↑ Brodland, David G.; Zitelli, John A. (1992). "Surgical margins for excision of primary cutaneous squamous cell carcinoma ". Journal of the American Academy of Dermatology 27 (2): 241–248. doi:. ISSN 01909622.
- ↑ 7.0 7.1 Monica Dahlgren, Janne Malina, Anna Måsbäck, Otto Ljungberg. Stora utskärningen. KVAST (Swedish Society of Pathology). Retrieved on 2019-09-26.
- ↑ 8.0 8.1 Katarzyna Lundmark. Handläggning av hudprover – provtagningsanvisningar, utskärningsprinciper och snittning (Handling of skin samples - sampling instructions, cutting principles and incision. Swedish Society of Pathology.
- ↑ Pathology Department at NU Hospital Group, Sweden, 2019-2020.
Image sources