Difference between revisions of "Endometrial polyp"
(→Microscopic evaluation: +Endoemtrial adenocarcinoma) |
(→Microscopic evaluation: EIN) |
||
| (9 intermediate revisions by the same user not shown) | |||
| Line 3: | Line 3: | ||
|author2= | |author2= | ||
}} | }} | ||
| + | {{Comprehensiveness}} | ||
{{Fixation - standard}} | {{Fixation - standard}} | ||
{{Fixation - general notes}} | {{Fixation - general notes}} | ||
| Line 13: | Line 14: | ||
*Look for signs of '''atypia or malignancy'''. | *Look for signs of '''atypia or malignancy'''. | ||
<gallery mode=packed heights=200> | <gallery mode=packed heights=200> | ||
| − | File:Histopathology of non-complex endometrial polyp without atypia.jpg|''' | + | File:Histopathology of non-complex endometrial polyp without atypia.jpg|'''Endometrial polyp''' (without atypia), with a thick-walled blood vessel in middle - typical of endometrial polyps. Glands are regular. |
| − | File:Histopathology of non-complex endometrial polyp without atypia, with tubal metaplasia.jpg|''' | + | File:Histopathology of non-complex endometrial polyp without atypia, with tubal metaplasia.jpg|'''Endometrial polyp''' (without atypia), with tubal metaplasia (black arrow, showing ciliated epithelium) and a thick-walled blood vessel (white arrow). The stroma is hemorrhagic in this case. |
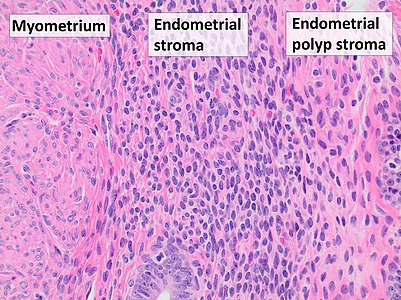
| − | File: | + | File:Myometrium versus endometrial stroma versus endometrial polyp stroma.jpg|Myometrium (smooth muscle cells) versus endometrial stroma (more cellular) versus '''endometrial polyp stroma''' (more collagenous).{{MH}} |
| − | File:Histopathology of | + | File:Histopathology of endometrial intraepithelial neoplasia (EIN).jpg|'''Atypia''' (mainly seen as signs of '''endometrial intraepithelial neoplasia''' ('''EIN'''), which has the following criteria:<ref name="OwingsQuick2014">{{cite journal|last1=Owings|first1=Richard A.|last2=Quick|first2=Charles M.|title=Endometrial Intraepithelial Neoplasia|journal=Archives of Pathology & Laboratory Medicine|volume=138|issue=4|year=2014|pages=484–491|issn=1543-2165|doi=10.5858/arpa.2012-0709-RA}}</ref><br>- Architectural gland crowding<br>- Altered cytology relative to background glands<br>- Minimum size of 1 mm<br>- Exclusion of adenocarcinoma<br>- Exclusion of mimics<br>Mitoses should also preferably be seen. |
| − | File:Histopathology of | + | File:Histopathology of Serous carcinoma arising in endometrial polyp.jpg|'''[[Endometrial adenocarcinoma]]'''<ref>{{cite journal|last1=Stewart|first1=Colin J.R.|last2=Crum|first2=Christopher P.|last3=McCluggage|first3=W. Glenn|last4=Park|first4=Kay J.|last5=Rutgers|first5=Joanne K.|last6=Oliva|first6=Esther|last7=Malpica|first7=Anais|last8=Parkash|first8=Vinita|last9=Matias-Guiu|first9=Xavier|last10=Ronnett|first10=Brigitte M.|title=Guidelines to Aid in the Distinction of Endometrial and Endocervical Carcinomas, and the Distinction of Independent Primary Carcinomas of the Endometrium and Adnexa From Metastatic Spread Between These and Other Sites|journal=International Journal of Gynecological Pathology|volume=38|year=2019|pages=S75–S92|issn=0277-1691|doi=10.1097/PGP.0000000000000553}}<br>- "Figures - available via license: Creative Commons Attribution 4.0 International"</ref> arising in an endometrial polyp. These are most commonly endometrioid, in which case low-grade carcinoma is distinguished from hyperplasia with atypia by the presence of glandular crowding with endometrial stromal exclusion, and significant cribriform, confluent glandular, labyrinthine, papillary/villoglandular, or non-squamous solid architecture.<ref name="RabbanGilks2019">{{cite journal|last1=Rabban|first1=Joseph T.|last2=Gilks|first2=C. Blake|last3=Malpica|first3=Anais|last4=Matias-Guiu|first4=Xavier|last5=Mittal|first5=Khush|last6=Mutter|first6=George L.|last7=Oliva|first7=Esther|last8=Parkash|first8=Vinita|last9=Ronnett|first9=Brigitte M.|last10=Staats|first10=Paul|last11=Stewart|first11=Colin J.R.|last12=McCluggage|first12=W. Glenn|title=Issues in the Differential Diagnosis of Uterine Low-grade Endometrioid Carcinoma, Including Mixed Endometrial Carcinomas|journal=International Journal of Gynecological Pathology|volume=38|year=2019|pages=S25–S39|issn=0277-1691|doi=10.1097/PGP.0000000000000512}}</ref> |
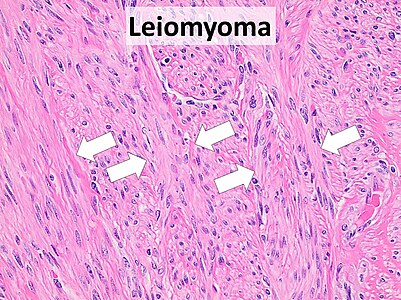
| − | File:Histopathology of | + | File:Histopathology of a leiomyoma with fascicular growth.jpg|Subserosal pedunculated uterine '''leiomyomas''' may present as endometrial polyps. They typically show smooth muscle in a fascicular pattern<ref>{{cite web|url=http://www.pathologyoutlines.com/topic/uterusleiomyoma.html|title=Uterus - Stromal tumors - Leiomyoma|author=Mohamed Mokhtar Desouki|website=pathology Outlines}} Topic Completed: 1 August 2011. Revised: 15 December 2019</ref> {{further|Smooth muscle tumor|linebreak=no}} |
</gallery> | </gallery> | ||
==Reporting== | ==Reporting== | ||
Most importantly: | Most importantly: | ||
| − | * | + | *Benign versus malignant {{Moderate-begin}}or presence or absence of atypia.{{Moderate-end}} |
| − | + | *{{Comprehensive-begin}}The size of the polyp.{{Comprehensive-end}} | |
| + | *{{Comprehensive-begin}}The type of epithelium at both the surface and gland coverings.{{Comprehensive-end}} | ||
| + | |||
| + | Example of a minimal report: | ||
| + | {|class=wikitable | ||
| + | | Benign endometrial polyp. | ||
| + | |} | ||
{{Reporting}} | {{Reporting}} | ||
{{Bottom}} | {{Bottom}} | ||
Latest revision as of 22:51, 8 August 2022
Author:
Mikael Häggström [note 1]
Contents
Comprehensiveness
On this resource, the following formatting is used for comprehensiveness:
- Minimal depth
- (Moderate depth)
- ((Comprehensive))
Fixation
Generally 10% neutral buffered formalin.
See also: General notes on fixation
Microscopic evaluation
The main objectives are:
- Making a diagnosis of endometrioid polyp. An endometrial polyp may be diagnosed in the presence of 2 of the following 3:
- Thick-walled vessels
- Collagenous stroma
- Epithelium on at least 3 sides
- Look for signs of atypia or malignancy.
Myometrium (smooth muscle cells) versus endometrial stroma (more cellular) versus endometrial polyp stroma (more collagenous).[image 1]
Atypia (mainly seen as signs of endometrial intraepithelial neoplasia (EIN), which has the following criteria:[1]
- Architectural gland crowding
- Altered cytology relative to background glands
- Minimum size of 1 mm
- Exclusion of adenocarcinoma
- Exclusion of mimics
Mitoses should also preferably be seen.Endometrial adenocarcinoma[2] arising in an endometrial polyp. These are most commonly endometrioid, in which case low-grade carcinoma is distinguished from hyperplasia with atypia by the presence of glandular crowding with endometrial stromal exclusion, and significant cribriform, confluent glandular, labyrinthine, papillary/villoglandular, or non-squamous solid architecture.[3]
Subserosal pedunculated uterine leiomyomas may present as endometrial polyps. They typically show smooth muscle in a fascicular pattern[4] Further information: Smooth muscle tumor
Reporting
Most importantly:
- Benign versus malignant (or presence or absence of atypia.)
- ((The size of the polyp.))
- ((The type of epithelium at both the surface and gland coverings.))
Example of a minimal report:
| Benign endometrial polyp. |
See also: General notes on reporting
Notes
- ↑ For a full list of contributors, see article history. Creators of images are attributed at the image description pages, seen by clicking on the images. See Patholines:Authorship for details.
Main page
References
- ↑ Owings, Richard A.; Quick, Charles M. (2014). "Endometrial Intraepithelial Neoplasia ". Archives of Pathology & Laboratory Medicine 138 (4): 484–491. doi:. ISSN 1543-2165.
- ↑ Stewart, Colin J.R.; Crum, Christopher P.; McCluggage, W. Glenn; Park, Kay J.; Rutgers, Joanne K.; Oliva, Esther; Malpica, Anais; Parkash, Vinita; et al. (2019). "Guidelines to Aid in the Distinction of Endometrial and Endocervical Carcinomas, and the Distinction of Independent Primary Carcinomas of the Endometrium and Adnexa From Metastatic Spread Between These and Other Sites
". International Journal of Gynecological Pathology 38: S75–S92. doi:. ISSN 0277-1691.
- "Figures - available via license: Creative Commons Attribution 4.0 International" - ↑ Rabban, Joseph T.; Gilks, C. Blake; Malpica, Anais; Matias-Guiu, Xavier; Mittal, Khush; Mutter, George L.; Oliva, Esther; Parkash, Vinita; et al. (2019). "Issues in the Differential Diagnosis of Uterine Low-grade Endometrioid Carcinoma, Including Mixed Endometrial Carcinomas ". International Journal of Gynecological Pathology 38: S25–S39. doi:. ISSN 0277-1691.
- ↑ Mohamed Mokhtar Desouki. Uterus - Stromal tumors - Leiomyoma. pathology Outlines. Topic Completed: 1 August 2011. Revised: 15 December 2019
Image sources
- ↑ Image(s) by: Mikael Häggström, M.D. Public Domain
- Author info
- Reusing images