Difference between revisions of "Urinary bladder"
(→Gross reporting of transurethral resections: Expanded) |
(→Bladder cancer: Edema) |
||
| (7 intermediate revisions by the same user not shown) | |||
| Line 8: | Line 8: | ||
===Gross reporting of transurethral resections=== | ===Gross reporting of transurethral resections=== | ||
| − | *Generally submit all material.<ref group=notes>It may be sufficient to submit representative sections that include the muscular layer, if grossly identified. Yet, many departments require submission of the entire specimen regardless, so if unsure, that is the safe choice.</ref> | + | *Generally submit '''all''' material.<ref group=notes>It may be sufficient to submit representative sections that include the muscular layer, if grossly identified. Yet, many departments require submission of the entire specimen regardless, so if unsure, that is the safe choice.</ref> |
*Submit in tea bags or equivalent.<ref>Tissue from transurethral resections are generally very brittle and may escape the openings of a conventional cassette.</ref> | *Submit in tea bags or equivalent.<ref>Tissue from transurethral resections are generally very brittle and may escape the openings of a conventional cassette.</ref> | ||
| Line 17: | Line 17: | ||
===Microscopy=== | ===Microscopy=== | ||
| − | + | Mainly look for '''[[urothelial carcinoma]]''' (also called transitional cell carcinoma), which constitutes 95% of bladder cancers.<ref name=CancerCenter>{{Cite web|url=https://www.cancercenter.com/bladder-cancer/types/|title=Types of Bladder Cancer: TCC & Other Variants|website=CTCA|access-date=2018-08-10}}</ref> | |
| − | |||
| − | |||
| − | |||
| − | |||
<gallery mode=packed heights=200> | <gallery mode=packed heights=200> | ||
| − | File:Papillary urothelial carcinoma (low-grade), very high mag.jpg|'''Low grade''': Urothelium is thickened but only slightly atypical and has maintained polarity. | + | File:Papillary urothelial carcinoma (low-grade), very high mag.jpg|'''Low grade [[urothelial carcinoma]]''': Urothelium is thickened but only slightly atypical and has maintained polarity. |
| − | File:Papillary urothelial carcinoma ( | + | File:Papillary urothelial carcinoma (high-grade), very high mag.jpg|'''High grade [[urothelial carcinoma]]''': Loss of polarity and severe abnormal cytology. |
| − | + | File:Histopathology of inverted urothelial papilloma, high magnification.jpg|In contrast, an '''inverted urothelial papilloma''' has smooth surface with minimal to absent exophytic component, is well circumscribed with smooth base, and has no obvious infiltration and no/minimal cytologic atypia.<ref>{{cite web|url=https://www.pathologyoutlines.com/topic/bladderinvertedpapilloma.html|title=Bladder, ureter & renal pelvis - Urothelial neoplasms - noninvasive - Inverted urothelial papilloma|website=Pathology Outlines|author=Monika Roychowdhury}} Topic Completed: 1 December 2014. Minor changes: 3 December 2020</ref> | |
| − | |||
| − | File: | ||
| − | |||
</gallery> | </gallery> | ||
| − | + | Other possibilities: | |
<gallery mode=packed heights=200> | <gallery mode=packed heights=200> | ||
| − | File: | + | File:Histopathology of squamous cell carcinoma of the urinary bladder, low magnification.jpg|'''Squamous cell carcinoma''' of the urinary bladder. {{further|Urothelial versus squamous cell carcinoma|linebreak=no}} |
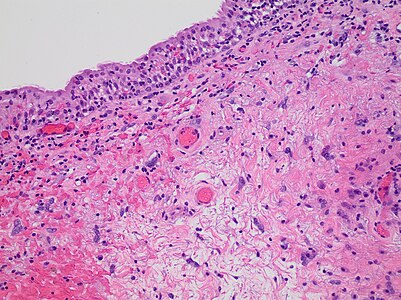
| − | File: | + | File:Histopathology of radiation cystitis.jpg|'''Radiation cystitis''' with atypical stromal cells (“radiation fibroblasts”), edema and inflammation. Check whether the patient has received radiation before making the diagnosis. |
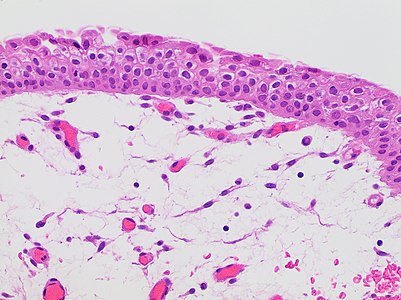
| − | + | File:Histopathology of non-specific urothelial edema.jpg|'''Edema''' (clear spaces of both the lamina propria and cytoplasm of multiple urothelial cells), which is non-specific. | |
| − | File: | ||
</gallery> | </gallery> | ||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
| − | |||
{{Bottom}} | {{Bottom}} | ||
Revision as of 09:13, 27 September 2021
Author:
Mikael Häggström [note 1]
Contents
Bladder cancer
The main condition of interest in urinary bladder cytologies and biopsies is bladder cancer.
Gross reporting of transurethral resections
Example report:
| Container A. Labeled "bladder tumor". The specimen is received in formalin and consists of multiple fragments of tan-gray, friable soft tissue measuring about __ x __ x __ cm in aggregate. The specimen is entirely submitted for microscopic examination in __ cassettes. |
Microscopy
Mainly look for urothelial carcinoma (also called transitional cell carcinoma), which constitutes 95% of bladder cancers.[2]
Low grade urothelial carcinoma: Urothelium is thickened but only slightly atypical and has maintained polarity.
High grade urothelial carcinoma: Loss of polarity and severe abnormal cytology.
In contrast, an inverted urothelial papilloma has smooth surface with minimal to absent exophytic component, is well circumscribed with smooth base, and has no obvious infiltration and no/minimal cytologic atypia.[3]
Other possibilities:
Squamous cell carcinoma of the urinary bladder. Further information: Urothelial versus squamous cell carcinoma
Notes
- ↑ It may be sufficient to submit representative sections that include the muscular layer, if grossly identified. Yet, many departments require submission of the entire specimen regardless, so if unsure, that is the safe choice.
- ↑ For a full list of contributors, see article history. Creators of images are attributed at the image description pages, seen by clicking on the images. See Patholines:Authorship for details.
Main page
References
- ↑ Tissue from transurethral resections are generally very brittle and may escape the openings of a conventional cassette.
- ↑ . Types of Bladder Cancer: TCC & Other Variants. CTCA.
- ↑ Monika Roychowdhury. Bladder, ureter & renal pelvis - Urothelial neoplasms - noninvasive - Inverted urothelial papilloma. Pathology Outlines. Topic Completed: 1 December 2014. Minor changes: 3 December 2020
Image sources