Neuroendocrine tumors of the midgut
Author:
Mikael Häggström [note 1]
The processing of neuroendocrine tumors (NET) of the midgut includes:
- Gross processing
- Microscopic evaluation
- Immunohistochemistry
- For diagnosis if not clear from initial microscopy
- Grading
Contents
Gross processing
Microscopic evaluation
Characteristics:[1]
- Round regular nuclei
- Stippled to granular (salt and pepper) chromatin
- Moderate to abundant cytoplasm
Diagnostic immunohistochemistry
If the diagnosis is not clear from light microscopy:
Synaptophysin: positive in almost all cases,[1] and is generally enough for confirmation.
Chromogranin: mostly positive[1]
Grading
Neuroendocrine lesions are graded histologically according to markers of cellular proliferation, rather than cellular polymorphism. For this purpose, it is recommended that mitotic count and Ki-67 index is determined for all gastroenteropancreatic neuroendocrine neoplasms:[2]
| G | Mitotic count (per mm2) | Ki-67 index (%) |
|---|---|---|
| GX | Grade cannot be assessed | |
| G1 | < 1 | < 3% |
| G2 | 1 to 10 | 3% - 20% |
| G3 | > 10 | > 20% |
Mitotic count
The mitotic count should be estimated by counting mitoses over 8 mm2 (or more), and then dividing that count by 8 (or proportionally more for a larger area).[3] Further information: Evaluation#Counts per mm2
Ki-67 index
The counting is made in areas with the highest concentration of Ki-67 positive cells, called "hot spots".[4]
The main methods are:
- 'Eye-balling' , which is apparently the most common method for determining the Ki-67 index. In 'eye-balling', an impression is made without actually counting individual cells. It can be done on one single view intermediate power (× 10 objective), or by scrolling at higher magnification.[4]
- Manual counting, which is indicated if eye-balling is within a factor of 2 from any grading limit (such as between 1.5% and 6%). It should be done by photographing (and perhaps printing) the slide so that cells can be marked as they are counted.[4] Officially, at least 500 cells should be counted.[5]
If the mitotic count and Ki-67 index are discordant, the figure which gives the highest grade is used.
G1 and G2 neuroendocrine neoplasms are called neuroendocrine tumors (NETs).[notes 1] G3 neoplasms are called neuroendocrine carcinomas (NECs).
Stage
Use the AJCC standard, and take both gross and microscopic evaluation into account:[6]
| Primary Tumor (T) | |
|---|---|
| T Category | Tumor Criteria |
| TX | Primary tumour cannot be assessed |
| T0 | No evidence of primary tumour |
| T1 | Invades the lamina propria or submucosa, and less than or equal to 1 cm in size |
| T2 | Invades the muscularis propria, or greater than 1 cm in size |
| T3 | Invades through the muscularis propria into subserosal tissue without penetration of overlying serosa |
| T4 | Invades visceral peritoneum (serosal) or other organs or adjacent structures |
| Regional Lymph Node (N) | |
| N Category | N Criteria |
| NX | Regional lymph nodes cannot be assessed (including no lymph nodes submitted or found) |
| N0 | No regional lymph node metastasis |
| N1 | Regional lymph node metastasis less than 12 nodes |
| N2 | Large mesenteric masses (> 2 cm) and / or extensive nodal deposits (12 or greater), especially those that encase the superior mesenteric vessels |
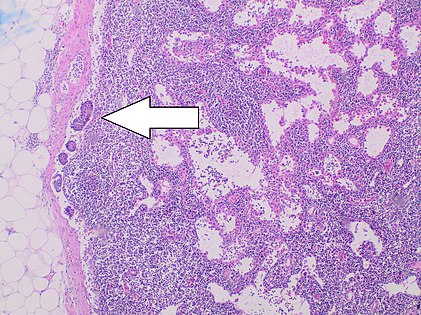
Mesenteric lymph node metastasis from neuroendocrine tumors of the midgut:
Report
It should include:
- Diagnosis of neuroendocrine tumor
- Grade
- T and N stage by AJCC standard
- Whether the resection is radical
Notes
- ↑ Neuroendocrine tumors of the intestines were formerly called carcinoid tumours
- ↑ For a full list of contributors, see article history. Creators of images are attributed at the image description pages, seen by clicking on the images. See Patholines:Authorship for details.
Main page
References
- ↑ 1.0 1.1 1.2 . Carcinoid / Well Differentiated Neuroendocrine Neoplasm / Tumor of the Ileum, Distal Jejunum and Cecum. Stanford University School of Medicine. Retrieved on 2022-06-18.
- ↑ >WHO Classification of Tumours of the Digestive System (4 ed.). Lyon: International Agency for Research on Cancer. 2010. pp. 13–14. ISBN 978-92-832-2432-7.
- ↑ First reference states 40 high power fields (HPFs) and second reference states that one HPF can be assumed to be 0.2 mm2:
-Rindi, G.; Klöppel, G.; Alhman, H.; Caplin, M.; Couvelard, A.; de Herder, W. W.; Erikssson, B.; Falchetti, A.; et al. (2006). "TNM staging of foregut (neuro)endocrine tumors: a consensus proposal including a grading system ". Virchows Archiv 449 (4): 395–401. doi:. ISSN 0945-6317.
- Klimstra, David S.; Modlin, Irvin R.; Coppola, Domenico; Lloyd, Ricardo V.; Suster, Saul (2010). "The Pathologic Classification of Neuroendocrine Tumors ". Pancreas 39 (6): 707–712. doi:. ISSN 0885-3177. - ↑ 4.0 4.1 4.2 Reid, Michelle D; Bagci, Pelin; Ohike, Nobuyuki; Saka, Burcu; Erbarut Seven, Ipek; Dursun, Nevra; Balci, Serdar; Gucer, Hasan; et al. (2014). "Calculation of the Ki67 index in pancreatic neuroendocrine tumors: a comparative analysis of four counting methodologies ". Modern Pathology 28 (5): 686–694. doi:. ISSN 0893-3952.
- ↑ Basile, Maíra Leite; Kuga, Fábio Seiji; Del Carlo Bernardi, Fabíola (2019). "Comparation of the quantification of the proliferative index KI67 between eyeball and semi-automated digital analysis in gastro-intestinal neuroendrocrine tumors ". Surgical and Experimental Pathology 2 (1). doi:. ISSN 2520-8454.
- ↑ Amin, Mahul (2017). AJCC cancer staging manual
(8 ed.). Switzerland: Springer. ISBN 978-3-319-40617-6. OCLC 961218414. Chapter: 29 - Neuroendocrine Tumors of the Stomach.
- For access, see the Secrets chapter of Patholines.
- Copyright note: The AJCC, 8th Ed. is published by a company in Switzerland, and the tables presented therein are Public Domain because they consist of tabular information without literary or artistic innovation, and therefore do not fulfil the inclusion criterion of the Swiss Copyright Act (CopA) which applies to "literary and artistic intellectual creations with individual character" (see Federal Act on Copyright and Related Rights (Copyright Act, CopA) of 9 October 1992 (Status as of 1 January 2022)).
Image sources