Template:Table comparing dermal nevus and suspected invasive melanoma
Jump to navigation
Jump to search
| Parameter | Non-dysplastic dermal nevus | Low-grade dysplastic dermal nevus | High-grade dysplastic dermal nevus | Suspected invasive melanoma | ||
|---|---|---|---|---|---|---|
| Mild dysplasia | Moderate dysplasia | Severe dysplasia | ||||
| Macroscopic | Lateral circumscription[1] | Sharp | Slightly diminished | Moderate | Poor | |
| Symmetry[1] | Good | Often broken | Rare | |||
| Structural (Low mag.) |
Micrograph |  |
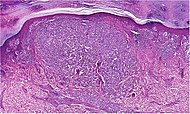
| |||
| Delimitation[2] | Rarely diffuse | Sometimes diffuse | Often diffuse | |||
| Confluent nests[2] | Rarely | Sometimes | Often | Often widespread | ||
| Pigment distribution[2] | Regular | Irregular | ||||
| Concentric fibrosis | Regressive (see below table)[1] | Yes[2] | Occasional[1] | |||
| Lamellar fibrosis | Rarely[2] | Often[2] | Often pronounced[2] | Occasional[1] | ||
| Lymphocytic infiltrate[2] | Mild, perivascular | Mild or moderate, perivascular | Varying | Varying | ||
| Cellular (high mag.) |
Micrographs | 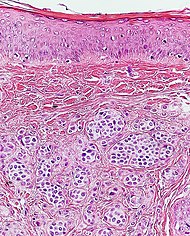 |

| |||
| Nuclear size[1] | Small | Medium | Large | Medium or large. Pleomorphic[3] | ||
| Nuclear pleomorphism[4] | Slight superficial | Slight | Prominent | |||
| Chromatin pattern | Uniform[1] | Condensed[1] | Partically expanded[1] | Expanded, coarse in some cells[1] | Expanded, hyperchromatic, coarse.[1] Usually granular.[4] | |
| Nucleoli[1] | Small | Medium | Large | Usually[4] large | ||
| Mitoses[1] | Few superficial | Superficial and deep | ||||
| Histological regression[4] (see below table) | Usually | Usually not | ||||
| Percentage of atypical melanocytes[2] | <10% | About 10 - 50% | about 50-90% | Usually> 90% | ||
Histological regression is one or more areas within a tumor in which neoplastic cells have disappeared or decreased in number. In this case, it means complete or partial disappearance of neoplastic cells from areas of the dermis (and occasionally from the epidermis), which have been replaced by fibrosis, accompanied by melanophages, new blood vessels, and a variable degree of inflammation.[5]
In suspected but not certain nevus or melanoma, generally perform immunohistochemistry with SOX10 (which stains cell nuclei of melanocytes), whereby melanocyte proliferation and nuclear pleomorphism is easier to see:[6]
See also
Notes
Main page
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 Arumi-Uria, Montserrat; McNutt, N Scott; Finnerty, Bridget (2003). "Grading of Atypia in Nevi: Correlation with Melanoma Risk ". Modern Pathology 16 (8): 764–771. doi:. ISSN 0893-3952.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Katarzyna Lundmark, Britta Krynitz, Ismini Vassilaki, Lena Mölne, Annika Ternesten Bratel. Histopatologisk bedömning och gradering av dysplastiskt nevus samt gränsdragning mot melanom in situ/melanom (Histopathological assessment and grading of dysplastic nevus and distinction from melanoma in situ/melanoma). KVAST (Swedish Society of Pathology). Retrieved on 2019-09-18.
- ↑ Christopher S. Hale. Skin melanocytic tumor - Melanoma - Invasive melanoma. Topic Completed: 1 May 2013. Revised: 17 September 2019
- ↑ 4.0 4.1 4.2 4.3 Husain, Ehab A; Mein, Charles; Pozo, Lucia; Blanes, Alfredo; Diaz-Cano, Salvador J (2011). "Heterogeneous topographic profiles of kinetic and cell cycle regulator microsatellites in atypical (dysplastic) melanocytic nevi ". Modern Pathology 24 (4): 471–486. doi:. ISSN 0893-3952.
- ↑ Ribero, Simone; Gualano, Maria Rosaria; Osella-Abate, Simona; Scaioli, Giacomo; Bert, Fabrizio; Sanlorenzo, Martina; Balagna, Elena; Fierro, Maria Teresa; et al. (2015). "Association of Histologic Regression in Primary Melanoma With Sentinel Lymph Node Status ". JAMA Dermatology 151 (12): 1301. doi:. ISSN 2168-6068.
- ↑ Miettinen, Markku; McCue, Peter A.; Sarlomo-Rikala, Maarit; Biernat, Wojciech; Czapiewski, Piotr; Kopczynski, Janusz; Thompson, Lester D.; Lasota, Jerzy; et al. (2015). "Sox10—A Marker for Not Only Schwannian and Melanocytic Neoplasms But Also Myoepithelial Cell Tumors of Soft Tissue ". The American Journal of Surgical Pathology 39 (6): 826–835. doi:. ISSN 0147-5185.
Image sources

